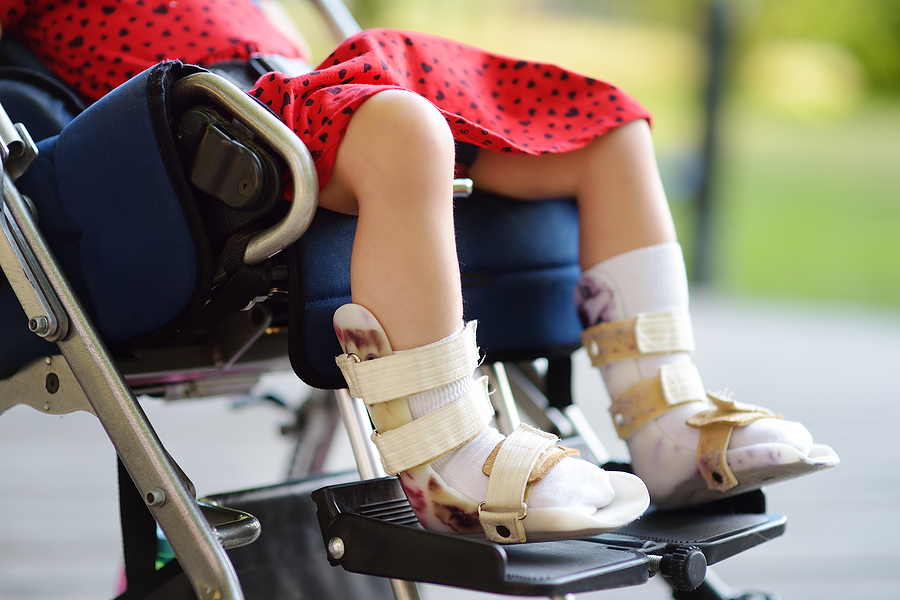
Abuse of Children With Disabilities in Residential Facilities
Children with disabilities in residential and therapeutic facilities are among those who are most vulnerable to abuse and other forms of harm. Protecting the safety of children and the facilities where they reside from costly litigation is achievable through proper policies, training, supervision of staff and students, and continued proactive...